What is Lyme Arthritis?
Lyme disease was first recognized in the United States in the 1970s, presenting as joint swelling (arthritis) during an outbreak in children in Lyme, Connecticut. It is now the most common vector-borne illness in North America and Europe.
The clinical manifestations of Lyme disease are divided into three phases:
- Early localized
- Early disseminated
- Late disease
Lyme disease can affect multiple organs, including the joints, resulting in what is termed Lyme arthritis. Lyme arthritis is the most common manifestation of late Lyme disease, occurring months to years after the exposure to B. burgdorferi, the causative agent of Lyme disease.
Lyme Arthritis Symptoms
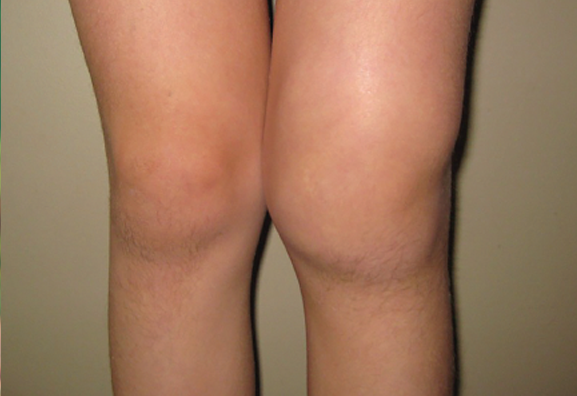
Lyme arthritis is characterized by the following symptoms:
- joint swelling
- redness
- warmth, most commonly involving a single knee
Other joints commonly impacted by Lyme arthritis include the shoulder, ankle, elbow, and wrist, which are typically involved in an asymmetric pattern. Almost always, fewer than five joints are involved (including the knee).
Lyme arthritis is not particularly painful, except due to pressure from a tensely swollen joint. Episodes of joint swelling tend to begin suddenly and may last for several weeks to months.
Diagnosis
Lyme disease blood testing is used to establish the diagnosis of Lyme arthritis in patients with potential exposure to Ixodes ticks, and those showing signs and symptoms consistent with Lyme arthritis.
Because Lyme arthritis is a late manifestation of Lyme disease, all patients with Lyme arthritis will have a positive blood test for Lyme (B. burgdorferi). Thus, those with negative blood tests are unlikely to have Lyme arthritis. B. burgdorferi DNA is detectable in joint fluid by polymerase chain reaction (PCR) in most patients with untreated Lyme arthritis; however, PCR testing of joint fluid has not been validated for widespread clinical use.
Lyme Arthritis Treatment
Because antibiotic treatment of early Lyme infection is usually curative, arthritic complications have become less common.
Studies of the natural history of Lyme arthritis demonstrate eventual resolution, even in the absence of antibiotic therapy. In most cases, however, the arthritis can last for years in untreated patients. Because of this, the current recommendation for treatment of Lyme arthritis is antibiotic therapy to accelerate the resolution of arthritis and prevent recurrence.
In 90% of patients with Lyme arthritis, 28 days of oral antibiotics (doxycycline or amoxicillin) will result in resolution of symptoms. Occasionally, a second course of the same oral antibiotic, or a longer course of intravenous antibiotics, may be required.